Neuropathy and Myopathy
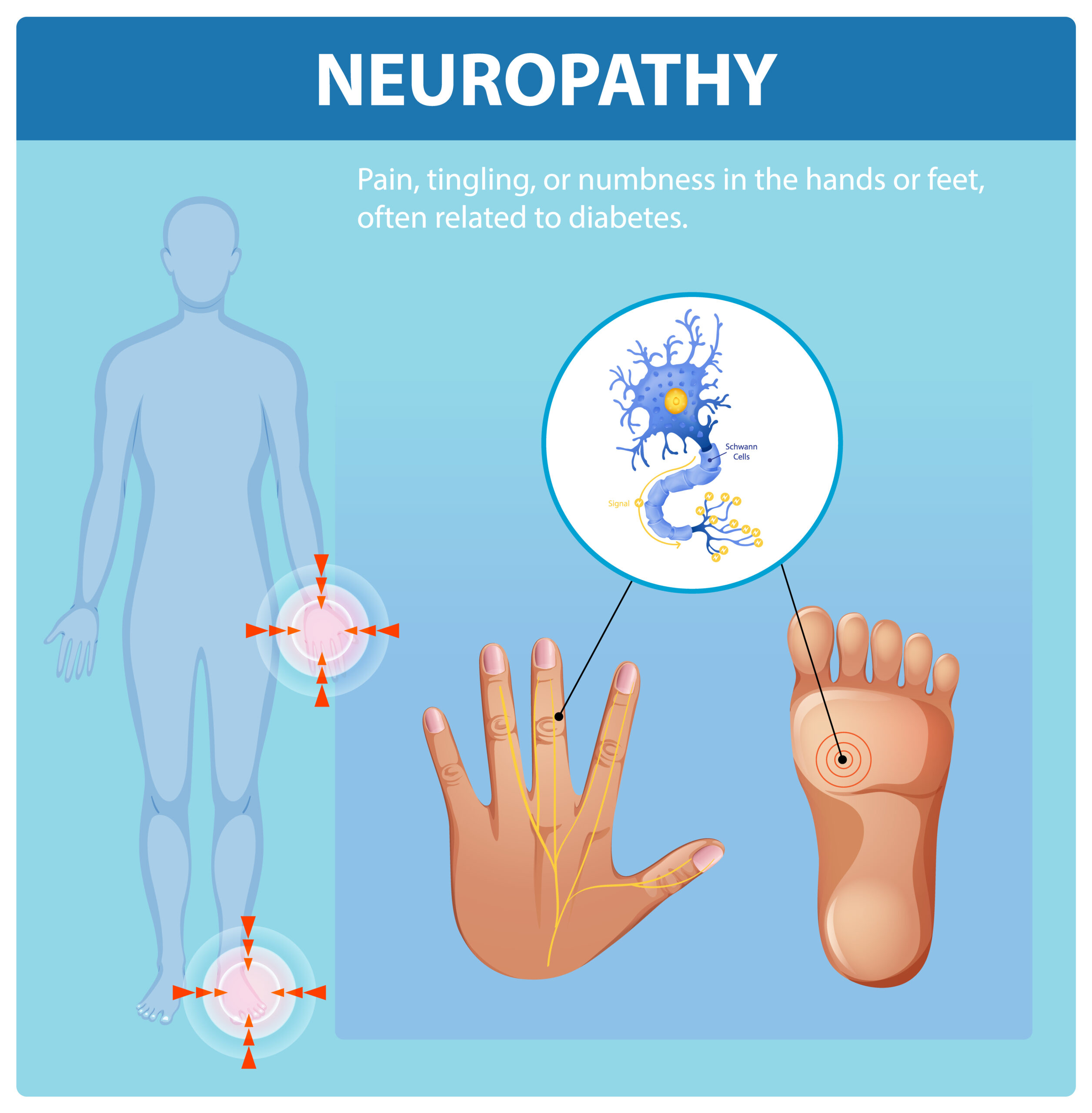
Neuropathy and Myopathy: Understanding Nerve and Muscle Disorders
What Are Neuropathy and Myopathy?
Neuropathy and myopathy are two different conditions affecting your nervous system, but they often have similar symptoms. Understanding which condition you have is crucial for proper treatment. The good news? Both conditions can be managed effectively with proper diagnosis and care, and many people improve significantly with appropriate treatment.
Neuropathy is disease of the peripheral nerves (nerves outside the brain and spinal cord). Myopathy is disease of the muscles themselves. Though different, they sometimes occur together and require expert evaluation to distinguish.
Neuropathy: Understanding Nerve Damage
What Is Peripheral Neuropathy?
According to HealthDirect Australia, neuropathy is a condition affecting the peripheral nerves that carry signals between your brain, spinal cord, and the rest of your body. When nerves are damaged, messages don’t travel correctly, causing various symptoms.
Think of it like damaged telephone wires – the signals (messages) can’t travel properly from your brain to your body parts.
Types of Neuropathy
| Type | Details |
|---|---|
| Sensory Neuropathy | Affects nerves carrying sensation (feeling, touch) |
| Motor Neuropathy | Affects nerves controlling muscle movement |
| Autonomic Neuropathy | Affects nerves controlling involuntary functions (heart rate, digestion) |
| Mixed Neuropathy | Combination of sensory, motor, and autonomic involvement |
Common Causes of Neuropathy
Medical Conditions:
| Cause | How It Damages Nerves |
|---|---|
| Diabetes (Most Common) | High blood sugar damages nerve fibers over time |
| Infections | Viral or bacterial infections (HIV, hepatitis C, Lyme) |
| Autoimmune Disorders | Body’s immune system attacks nerve tissue |
| Cancer & Chemotherapy | Chemotherapy drugs damage nerve cells |
| Liver/Kidney Disease | Toxic buildup damages peripheral nerves |
| Hypothyroidism | Thyroid hormone deficiency affects nerve function |
Other Causes:
✓ Nutritional deficiencies – B vitamins, copper deficiency
✓ Alcoholism – Toxic effects on nerves
✓ Toxin exposure – Industrial chemicals, heavy metals
✓ Medication side effects – Some drugs can cause neuropathy
✓ Injury or trauma – Physical damage to nerves
✓ Idiopathic – Unknown cause (about 1/3 of cases)
Symptoms of Neuropathy
According to HealthDirect, symptoms depend on which type of nerves are affected:
Sensory Symptoms:
Numbness or tingling (often starts in feet/hands)
Burning sensation
Electric shock-like sensations
Increased sensitivity to light touch
Difficulty feeling temperature changes
Loss of balance or coordination
Motor Symptoms:
Weakness in hands, arms, legs, or feet
Difficulty with fine movements (buttoning, writing)
Muscle twitching or cramping
Difficulty walking or climbing stairs
Autonomic Symptoms:
Abnormal sweating
Heart rate irregularities
Dizziness or lightheadedness
Digestive problems
Myopathy: Understanding Muscle Disease
What Is Myopathy?
Myopathy refers to disease of the muscles themselves. According to the Muscular Dystrophy Association, myopathies can be genetic, inflammatory, metabolic, or toxic in origin.
Think of it like defective engine parts – the muscles themselves aren’t working properly rather than the signals being disrupted.
Types of Myopathy
| Type | Characteristics |
|---|---|
| Inflammatory Myopathy | Immune system attacks muscle fibers |
| Muscular Dystrophy | Genetic muscle degeneration (Duchenne, Becker) |
| Metabolic Myopathy | Energy production problem in muscles |
| Toxic Myopathy | Medication or substance damage to muscles |
| Endocrine Myopathy | Hormonal dysfunction affecting muscles |
Polymyositis: Common Inflammatory Myopathy
According to Rare Diseases Organization, polymyositis (PM) is an inflammatory myopathy where immune cells attack muscle fibers:
| Feature | Details |
|---|---|
| What happens | Immune system directly attacks muscle fiber cells |
| Typical onset | After age 20, usually in adults |
| Progression | Gradual weakening over weeks to months |
| Muscles affected | Hip, shoulders, arms, neck, throat (near trunk) |
| Hand/face involvement | Rarely affected (unlike some other myopathies) |
| Associated symptoms | Possible muscle pain, breathing difficulty, swallowing issues |
| Good news | Effective treatments available, many recover partially or fully |
Symptoms of Myopathy
Primary Muscle Symptoms:
Weakness in proximal muscles (shoulders, hips, neck)
Difficulty rising from chair or climbing stairs
Trouble lifting arms overhead
Neck weakness (difficulty holding head up)
Facial or throat weakness
Secondary Symptoms:
Muscle pain or soreness
Muscle cramping
Fatigue
Difficulty swallowing (dysphagia)
Breathing problems (if respiratory muscles affected)
Falls due to weakness
Progression:
Usually gradual (weeks to months)
May fluctuate over time
Muscle wasting (atrophy) may develop
Key Differences: Neuropathy vs. Myopathy
| Characteristic | Neuropathy | Myopathy |
|---|---|---|
| What’s affected | Peripheral nerves | Muscle fibers themselves |
| Typical pattern | Often starts in feet/hands | Starts in proximal muscles |
| Weakness location | Distal (hands, feet) | Proximal (shoulders, hips, neck) |
| Reflexes | Often decreased or absent | Usually normal |
| Muscle atrophy | Occurs later | More prominent early |
| Sensory loss | Common | Uncommon |
| Diagnostic test | EMG/NCS | Muscle biopsy, elevated enzymes |
Chemotherapy-Induced Neuropathy: Special Consideration
For cancer patients, chemotherapy-induced peripheral neuropathy (CIPN) is a major concern. According to research:
Common Chemotherapy Drugs Causing Neuropathy:
| Drug Class | Drugs | Neuropathy Risk |
|---|---|---|
| Taxanes | Paclitaxel, Docetaxel | 15-60% of patients |
| Platinum Agents | Cisplatin, Oxaliplatin | 14-94% (varies by dose) |
| Vinca Alkaloids | Vincristine, Vinorelbine | 44-60% incidence |
| Antimetabolites | 5-FU, Gemcitabine | Lower risk (3-12%) |
Higher Risk in Diabetes:
Studies show diabetes increases CIPN risk significantly. Patients with diabetes who receive chemotherapy need extra monitoring and may develop more severe neuropathy.
Warning Signs: When to Seek Help
Symptoms That Warrant Medical Evaluation
According to HealthDirect Australia, see your doctor if you experience:
✓ Numbness or tingling
✓ Burning or electric shock sensations
✓ Weakness or difficulty with coordination
✓ Extra sensitivity to light touch
✓ Changes in these symptoms
When to See a Neurologist
According to Houston Methodist, you should see a neurologist if you have:
Chronic numbness or tingling
Progressive muscle weakness
Difficulty with balance or coordination
Unexplained muscle pain or cramping
Symptoms affecting daily activities
Symptoms persistent for more than 2 weeks
Getting Diagnosed
Neuropathy Diagnosis
Doctors use several approaches to evaluate neuropathy:
Clinical Evaluation:
Detailed symptom history
Physical examination (strength, sensation, reflexes)
Assessment of daily functioning
Diagnostic Testing:
| Test | What It Shows |
|---|---|
| Blood Tests | Diabetes, vitamin deficiencies, infections |
| Nerve Conduction Studies (NCS) | Measures how fast electrical signals travel along nerves |
| Electromyography (EMG) | Records muscle electrical activity, detects nerve/muscle damage |
| Skin Biopsy | Counts nerve fibers in skin |
| Imaging (MRI/CT) | Rules out nerve compression or tumors |
How EMG/NCS Works:
According to Johns Hopkins, NCS delivers mild electrical stimulation (like a strong static shock) while measuring nerve response. EMG inserts a thin needle into muscle to record electrical activity. The discomfort is minimal and brief.
Myopathy Diagnosis
Testing for myopathy includes:
Blood tests (elevated muscle enzymes like CK, aldolase)
Muscle biopsy (shows inflammation or damage)
EMG/NCS (different pattern than neuropathy)
Genetic testing (if inherited myopathy suspected)
MRI (shows muscle inflammation)
Treatment Approaches
Neuropathy Management
Treatment depends on the cause and severity. According to Cleveland Clinic:
Treating the Underlying Cause (When Possible):
Diabetes control – Tight blood sugar management
Vitamin supplementation – B vitamins, copper if deficient
Addressing infections – Appropriate antibiotics or antivirals
Medication adjustment – Change drugs causing neuropathy if possible
Toxin removal – Eliminate exposure to harmful substances
Symptom Management:
Pain relief – Over-the-counter or prescription pain medications
Topical treatments – Creams containing capsaicin or lidocaine
Medications – Gabapentin, pregabalin for nerve pain
Physical therapy – Exercises to maintain strength and balance
Supportive devices – Canes, walkers, special shoes
Myopathy Management
According to research on multidisciplinary myopathy management, treatment focuses on four areas:
| Strategy | Details |
|---|---|
| Strength Therapies | Medications (corticosteroids for inflammatory myopathies) |
| Supportive Care | Respiratory support if needed, nutrition, pain management |
| Symptomatic Therapies | Treat pain, fatigue, swallowing difficulties |
| Rehabilitation | Physical therapy improves function, low-intensity exercise |
Specific Treatments:
Inflammatory myopathy – Corticosteroids, immunosuppressants
Metabolic myopathy – Enzyme replacement or cofactor therapy
Genetic myopathy – Supportive care, emerging gene therapies
Exercise Considerations:
Aerobic exercise well-tolerated in inflammatory myositis
Low-intensity programs recommended (high-intensity not supported)
Benefits beyond strength: improved cardiopulmonary function, mood
Baseline strength assessment recommended before starting exercise
Prevention and Lifestyle Management
Neuropathy Prevention
For Diabetic Neuropathy Prevention:
Tight blood sugar control (most effective)
Regular exercise
Healthy diet rich in antioxidants
Foot care and inspection
Avoid smoking and excessive alcohol
Maintain healthy weight
For Chemotherapy Patients:
Discuss neuropathy risk with oncology team
Monitor symptoms closely during treatment
Maintain optimal nutrition
Avoid additional neurotoxic substances
Report symptoms early (may allow dose adjustment)
Living With Neuropathy or Myopathy
Safety Measures:
Wear protective footwear
Inspect feet daily for injuries
Improve home lighting
Install handrails and grab bars
Use mobility aids if needed
Symptom Management:
Maintain consistent activity level
Manage pain effectively
Address sleep problems
Join support groups
Psychological support for chronic conditions
Frequently Asked Questions
Some causes are reversible if caught early (vitamin deficiency, certain infections). Others improve with treatment but don’t completely resolve. Diabetic neuropathy requires tight blood sugar control to prevent worsening.
Progression depends on the type. Inflammatory myopathies often respond well to treatment with partial or complete recovery. Genetic muscular dystrophies progress gradually. Many myopathies stabilize with appropriate management.
Treatment depends on the cause. Treatable causes (vitamin deficiency, infection, medication side effect) may be cured by addressing the underlying problem. Others can be managed to reduce symptoms and slow progression.
No. Muscular dystrophy is a type of genetic myopathy, but myopathy is broader – including inflammatory, metabolic, and toxic muscle diseases. Not all myopathies are inherited.
Simple cases may be diagnosed in days. Complex cases may take weeks for imaging, biopsies, and additional testing. EMG/NCS can be done quickly but need expert interpretation.
Yes, with proper guidance. Physical therapy is beneficial for both. Always work with your healthcare team to create a safe, appropriate exercise program.
Many conditions improve significantly with proper treatment and management. Some improvement is often possible even in chronic cases. Prognosis depends on the specific condition and severity.
According to Houston Methodist, yes if you have persistent numbness, weakness, pain, or coordination problems. A neurologist can properly diagnose and manage these conditions.
Your Next Steps with NeuroLogic Neurocare
Dr. Mohammed Imran Khan specializes in diagnosing and treating peripheral neuropathy and myopathy. Expert evaluation is crucial for accurate diagnosis and effective management.
Quick Links:
Early diagnosis matters. Proper identification and management can prevent progression and significantly improve your quality of life. Contact NeuroLogic Neurocare today to get a comprehensive neurological evaluation and personalized treatment plan.
Disclaimer:
This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. If you’re experiencing numbness, tingling, weakness, or other neurological symptoms, consult a qualified neurologist for proper evaluation and personalized care. Always discuss symptoms, treatment options, and medications with your healthcare provider.