Sciatica / Slipped Disc
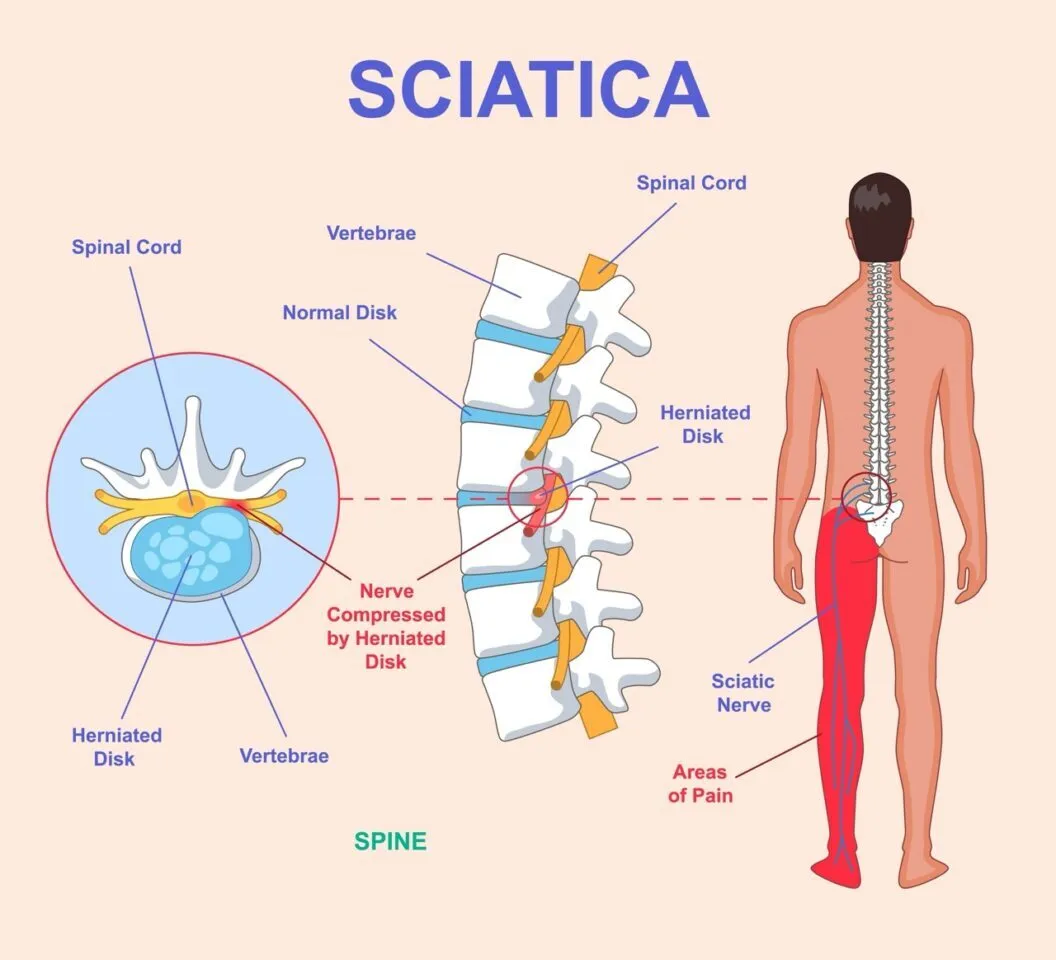
Sciatica and Slipped Disc: Understanding, Recovery, and Reclaiming Your Mobility
What Is Sciatica and Slipped Disc?
Sciatica is pain radiating along the sciatic nerve—the longest nerve in your body—typically caused by compression or irritation of the nerve root. A slipped disc (also called herniated, prolapsed, or ruptured disc) is when the inner gel of a spinal disc pushes through the outer layer, often compressing nearby nerve roots and causing sciatica. The good news? Most cases resolve with conservative treatment. About 90% of people improve significantly with physical therapy and proper management without surgery.
According to Patient.info, healing timelines are encouraging: 50% improve within 10 days, 75% within 4 weeks, and 90% within 6 weeks. Only about 2% require surgery because symptoms persist beyond 12 weeks.
Think of a slipped disc like a jelly donut with a crack—the jelly (nucleus pulposus) leaks out and presses on nearby nerves, causing pain that radiates down your leg. Understanding this mechanism helps explain both the pain and the recovery process.
Understanding the Spine and Discs
Normal Disc Structure
Your spinal discs are essential shock absorbers:
| Component | Function |
|---|---|
| Nucleus Pulposus | Gel-like center that absorbs impact and stress |
| Annulus Fibrosus | Tough outer layer containing the nucleus |
| Endplate | Connects disc to vertebral bodies above and below |
| Purpose | Allows movement, absorbs shock, maintains disc height |
What Happens With a Slipped Disc
According to Kauverya Hospitals, disc herniation progresses through stages:
| Stage | What Happens | Severity |
|---|---|---|
| Protrusion | Disc bulges out; outer layer remains intact | Mildest |
| Prolapse | Inner gel pushes through but remains contained | Moderate |
| Extrusion | Inner core breaks through and extends outside disc | Severe |
| Sequestration | Inner core fragments move entirely outside disc | Most Severe |
Symptoms: Recognizing Sciatica and Slipped Disc
Classic Sciatica Pain Pattern
According to Mass General, sciatica has a distinctive pattern:
Sharp, Shooting Pain:
Radiates from lower back through buttocks
Travels down one leg (usually one side)
Often described as electric shock or burning
May follow specific nerve pathway (thigh, calf, foot)
Nerve-Specific Symptoms:
L5 radiculopathy: Pain down outside of leg to top of foot
S1 radiculopathy: Pain down back of leg to sole of foot
Common Symptoms
✓ Pain and Sensation:
Sharp, radiating leg pain (worse than back pain)
Numbness or tingling (feet, legs, buttocks)
Burning sensation along nerve pathway
Electric shock sensations
✓ Weakness and Functional Loss:
Weakness in legs or feet
Difficulty walking or climbing stairs
Loss of ankle reflex
Foot drop (dragging foot while walking)
✓ Movement-Related Patterns:
Pain worsens with certain positions (prolonged sitting, bending forward)
Pain improves with walking or lying down
Coughing or sneezing makes pain worse
Relief often found with change of position
Red Flag Symptoms (Need Immediate Care)
🚨 Seek Emergency Care If:
Sudden loss of bowel or bladder control
Sudden numbness in genital area or buttocks
Severe progressive weakness in both legs
Signs of infection (fever with back pain)
These indicate cauda equina syndrome—a surgical emergency.
Causes: Why Discs Slip
Most Common Causes
According to Mass General Orthopaedics:
Disc Herniation (Most Common):
Disc material pressing on nerve root
Causes inflammation and nerve irritation
Can follow minor activity or happen gradually
Spinal Stenosis:
Narrowing of spinal canal
Can compress multiple nerves
Often develops with aging
Spondylolisthesis:
Vertebra slips forward over adjacent vertebra
Can compress nerve root
May be degenerative or developmental
Other Causes:
Degenerative disc disease (disc drying and shrinking)
Bone spurs from arthritis
Muscle tightness compressing nerve
Trauma or injury to spine
Risk Factors
✓ Lifestyle factors:
Prolonged sitting or sedentary lifestyle
Poor posture
Heavy lifting with poor technique
Repetitive bending or twisting
✓ Age and Health Factors:
Age 30-50 (higher risk)
Obesity
Smoking (reduces disc nutrition)
Previous back injury
Diagnosis: How Doctors Identify Your Problem
Clinical Evaluation
According to Physio-pedia, diagnosis includes:
Physical Examination:
Straight Leg Raise test – Positive test reproduces radiating pain
Slump test – Reproduces sciatica symptoms
Crossed Straight Leg Raise – Very specific for nerve compression
Neurological testing (reflexes, sensation, strength)
Palpation of spine and trigger points
Imaging and Tests
| Test | What It Shows |
|---|---|
| MRI (Gold Standard) | Clearly shows disc herniation and nerve compression [web:223] |
| X-Rays | Shows bone structure, degenerative changes, trauma |
| CT Scan | Alternative to MRI, good bone detail |
| EMG/NCS | Detects nerve damage and electrical patterns |
| Clinical Tests | Straight leg raise, neurological examination |
Recovery Timeline: When Will You Feel Better?
The Good News: Most Recover Quickly
According to rigorous research:
| Timeline | Recovery Rate |
|---|---|
| 10 days | 50% of patients significantly improved |
| 4 weeks | 75% improved or recovering well |
| 6 weeks | 90% have recovered substantially |
| 12 weeks | 98% resolved without surgery; only 2% need surgery |
Recovery Stages
According to spine health specialists:
Stage 1: Acute Inflammation (Days 1-2 weeks)
Maximum pain and symptoms
Rest and anti-inflammatory management
Avoid aggravating positions
Pain medications, ice, gentle movement
Stage 2: Gradual Improvement (Weeks 2-6)
Decreased pain intensity and frequency
Reduced muscle spasms
Improved range of motion
Less numbness or tingling
Return to gentle activity
Physical therapy becomes primary treatment
Stage 3: Plateau and Stabilization (Weeks 6-12)
Significant pain improvement
Occasional flare-ups possible
Progressive strengthening
Return to modified normal activities
Prevention focus
Stage 4: Long-Term Management (Beyond 12 Weeks)
Most resume normal activities
Focus on prevention and maintenance
Regular exercise and posture awareness
Avoid re-injury triggers
Treatment: The Path to Recovery
Conservative Treatment (First-Line Approach)
According to evidence-based research, conservative treatment is highly effective:
Effectiveness:
Better long-term quality of life outcomes
No surgical risks or complications
Recommended as initial approach
Physical Therapy: The Core of Treatment
According to Spine-Health, physical therapy is typically first-line treatment with eight key goals:
| Physical Therapy Goal | How It Helps |
|---|---|
| Pain Relief | Reduce sciatica and lower back pain |
| Reduce Spasms | Decrease involuntary muscle contractions |
| Restore Mobility | Improve range of motion and flexibility |
| Spine Restoration | Restore lumbar and sacroiliac joint function |
| Lower Body Mobility | Improve hip, thigh, and leg movement |
| Healing Environment | Foster optimal conditions for tissue healing |
| Pain Perception | Promote neurologic adaptations reducing pain sensation |
| Prevention | Reduce future flare-ups and fear of movement |
Specific Physical Therapy Techniques
The McKenzie Method (Mechanical Diagnosis and Therapy):
Series of active directional movements
Identifies specific pain source
Goal: centralize radiating pain toward spine
Highly effective for disc herniation
Specialized training required for therapists
Exercise Categories:
| Exercise Type | Examples and Benefits |
|---|---|
| Extension/Flexion | Backward/forward bending; promotes pain-relieving movement |
| Strengthening | Planks, bridges, resistance exercises for core/legs |
| Flexibility | Knee-to-chest stretches, hamstring stretches |
| Functional | Proper lifting, bending, squatting techniques |
| Gait Training | Corrected walking pattern with video analysis |
Sample Sciatica Exercises:
According to physical therapy experts, effective exercises include:
Knee-to-Chest Stretch (3 sets, 30 seconds each)
Lying on back, pull one knee toward chest
Hold 30 seconds, repeat 3 times per leg
Piriformis Stretch (Releases deep buttock muscle)
Lying on back, cross one leg over opposite knee
Pull knee toward chest, 30 seconds
Glute Bridges (Strengthening)
Lying on back, knees bent
Lift hips toward ceiling, hold 2 seconds
Repeat 10-15 times
Pelvic Tilts (Core activation)
Lying on back, tighten abdomen
Rock pelvis slightly, hold briefly
Repeat 10 times
Walking (Functional recovery)
Start with 5-10 minute walks
Gradually increase distance
Improves strength and flexibility
Important: Combined exercise AND manual therapy produces best outcomes vs. exercise alone. Start early for best results!
Other Conservative Treatments
Medications:
Over-the-counter NSAIDs (ibuprofen, naproxen)
Prescription pain relief if needed
Muscle relaxants for spasm reduction
Avoid long-term opioid use
Additional Therapies:
Epidural steroid injections (reduces inflammation)
Heat and ice application
Massage and manual therapy
Spinal traction (selective cases)
When Surgery Is Considered
According to research comparing surgical vs. conservative approaches, surgery is considered when:
Conservative treatment fails after 6-12 weeks
Severe neurological deficits develop
Cauda equina syndrome (emergency)
Progressive weakness or dysfunction
Surgical Options
| Procedure | Details |
|---|---|
| Microdiscectomy | Minimally invasive; small incision to remove disc material |
| Discectomy | Traditional open surgery; larger incision, more tissue damage |
| Laminectomy | Removes lamina to enlarge spinal canal; effective for stenosis |
| Laminotomy | Smaller version of laminectomy; more targeted decompression |
Microdiscectomy Advantages:
Smaller incision = less tissue trauma
Faster recovery than traditional surgery
Effective pain relief
Lower complication rates
Recovery After Surgery:
Hospitalization: Brief (same-day or overnight)
Avoid driving for 14+ days
Return to work: 2-4 weeks typically
Return to full activity: 6-8 weeks
Prevention: Staying Sciatica-Free
Daily Habits for Spine Health
✓ Posture and Mechanics:
Maintain good posture throughout day
Proper sitting posture (feet flat, back supported)
Correct lifting technique (bend knees, keep back straight)
Avoid prolonged sitting; take movement breaks hourly
✓ Activity and Exercise:
Regular moderate exercise (walking, swimming, yoga)
Core strengthening exercises 3-4x weekly
Flexibility and stretching routine
Avoid heavy lifting without proper form
✓ Lifestyle Factors:
Maintain healthy weight
Avoid smoking
Stay well-hydrated
Manage stress effectively
Sleep on supportive mattress
Ergonomic workstation setup
Frequently Asked Questions
Most people recover within 6 weeks with proper treatment. Some improve within days; others take weeks. Only 2% need surgery due to persistent symptoms beyond 12 weeks.
Brief rest (1-2 days) helps acute pain, but prolonged bed rest worsens outcomes. Early, gentle movement and progressive activity promotes faster healing through neuroplasticity.
Yes. Most cases resolve spontaneously with conservative management. The inflamed nerve gradually improves as pressure decreases and inflammation subsides.
Surgery is considered when conservative treatment fails after 6-12 weeks or if severe neurological deficits develop. Most cases resolve without surgery.
Avoid heavy lifting, excessive bending forward, high-impact activities (running, jumping), and positions that reproduce pain. A physical therapist personalizes exercise recommendations.
Yes, usually. After initial recovery (4-6 weeks), gradual return to sport is possible. Start with lower-impact activities, gradually progress. Proper technique and core strength prevent re-injury.
Yes. Walking is an excellent low-impact exercise for sciatica recovery. Start with short distances (5-10 minutes), gradually increase. It improves flexibility, strength, and cardiovascular health while being gentle on the nerve.
Risk of recurrence is 5-20%, depending on prevention efforts. Maintaining good posture, regular exercise, proper lifting technique, and core strength significantly reduce recurrence risk.
Your Next Steps with NeuroLogic Neurocare
Dr. Mohammed Imran Khan specializes in diagnosing and managing sciatica and slipped disc. Expert evaluation ensures accurate diagnosis and initiation of effective treatment to speed recovery.
Quick Links:
Sciatica and slipped discs are highly treatable. With proper diagnosis and evidence-based treatment, most people recover within weeks. Contact NeuroLogic Neurocare today to get a comprehensive evaluation, accurate diagnosis, and personalized treatment plan. Don’t live with radiating leg pain—relief is within reach.
Disclaimer:
This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. If you’re experiencing sciatica pain, numbness, or weakness, consult a qualified neurologist or spine specialist for proper evaluation and personalized care. Seek emergency medical attention for sudden loss of bladder/bowel control or severe progressive neurological symptoms.